Background and Objective: Recently, the first diode laser with a wavelength of 755 nm for in-motion hair removal came on the market. The objective of this study was to check its efficacy, safety, and practicality under different options for its use.
Methods: A prospective study in a heterogeneous group of 56 patients who had hair removed from various areas of their bodies using three different treatment methods. Four sessions were scheduled in all cases, with a gap of 3 months between each session. Efficacy was assessed by counting of hairs per cm2 and the adverse effects in each session were recorded in detail in the patients’ clinical histories. Results: The three tested options achieved a significant reduction in the number of hairs (P < 0.0001). The average clearances achieved using the conventional method (HR), the in-motion method (SHR) and the stacking method were 75.5%, 70.1%, and 41.9%, respectively. The degree of satisfaction of the participants on a scale of 0–10 was 7.7, 8.1, and 6.8, respectively. Erythema and perifollicular edema, which are characteristic responses in laser hair removal, were observed. The incidence of burns was 1.33%. Conclusion: The 755-nm diode laser performed efficiently and safely in all the tested areas, using high total accumulated energy per surface unit. Based on our prior experience with other equipment, the results are promising.
Key words: 755 nm; diode laser; hair removal; super hair removal; epilation; photoepilation
INTRODUCTION
Laser hair removal has emerged as a leading treatment option for long-term hair removal. The 755-nm long-pulse alexandrite and 810-nm long-pulse diode lasers present a better efficacy and safety profile, and are currently the most commonly used lasers for photoepilation. The choice of one or other laser depends on the color and thickness of the hair and the skin phototype. The main limitation of the 755-nm alexandrite laser is darker phototypes and the most significant limitation of the 810-nm diode laser is medium-fine hair types [1–6].
In August 2014, the Food and Drug Administration (FDA) approved the first 755-nm diode laser for medical hair removal. Its use is becoming more widespread in the USA and the European Union, where it is also authorized. According to unpublished research provided by the manufacturer, it enables more effective hair removal in all hair types and skin phototypes.
The only scientific study involving the new 755-nm diode laser is a single-case report of hair removal in a 47-year-old man, with Fitzpatrick skin phototype II and dark brown coarse hair. The patient was studied using a split-body methodology, where the hair was removed from his chest using the 755-nm diode laser in motion (non-conventional in-motion technique), from the right armpit with the 755-nm diode laser using the conventional technique, and from the left armpit using the 755-nm long-pulse alexan-drite laser. Hair removal levels of above 90% were achieved using the in-motion technique in just four sessions. Clearances of almost 90% were also achieved in four sessions using the conventional technique, compared to 77.7% achieved using the 755-nm alexandrite laser. The patient stated that the new diode was less painful than the traditional alexandrite laser [7].
Data on the efficacy and safety of the 755-nm diode laser in larger patient samples have not been reported, and no information is available on its use with darker skin phototypes. One of the main aspects that we attempted to clarify is whether the 755-nm diode laser, when used in its in-motion mode, can remove all hair types in darker phototypes, without the intrinsic predicted risks of the wavelength, which has a greater affinity for melanin.
MATERIALS AND METHODS
Study Design and Patient Characteristics
We designed the study based on our experience in this type of research [6], with prior knowledge of tolerated dosimetries and in compliance with the ethical principles of the Declaration of Helsinki. The trial was approved by the ethics committee of the Antoni de Gimbernat Founda-tion (Cambrils, Tarragona, Spain).
Sixty patients who attended the Instituto Medico Laser (Madrid, Spain) for medical hair removal were recruited, irrespective of the area from where the hair was to be removed or the skin phototype. The main inclusion criterion was the patients’ commitment to participate under the terms agreed through informed consent. Patients under 18 years of age were excluded, as were pregnant and lactating women, people with skin injuries in the area to be treated, patients with organic or psychiatric disorders that might interfere with results, and any patients that had used other hair removal methods in the previous 6 months. Patients were warned that, removal of the maximum number of hairs would involve a certain degree of pain, which was usually easy to tolerate without anesthetic.
A total of 56 subjects completed the study (18 men and 38 women), with an average age of 31.4 years (r =18–46 years), with Fitzpatrick phototypes of between II and V, and with black or brown hair of varying thicknesses and tones. The treated areas, depending on the individual cases, were the chest, abdomen, armpits, arms, legs, cervical area, back, lumbar area, bikini line, between the eyebrows, around the mouth, and beard. Of the three possible treatments offered by the new laser, 28 patients were treated using the conventional technique (Hair Removal, HR), 22 patients with the in-motion technique (Super Hair Removal, SHR) and six patients with the stacking technique (static hair removal in bursts). Of the 28 patients treated using the HR technique, 19 had never had hair removed before and nine had a history of prior hair removal using other equipment more than 6 months previously, with results that had not been sufficiently satisfactory. Of the 22 patients treated using the SHR technique, seven had a history of prior multiple hair-removal sessions with other lasers, without sufficient removal of fine or hypopigmented hair. None of the patients treated using the stacking technique had a history of prior hair removal. In terms of darker photo-types, 14 patients with phototype IV and three patients with phototype V were treated using the in-motion technique, including cases with fine and/or slightly pigmented hair.
All of the areas were treated in four sessions, with a gap of 3 months between each session. The results were assessed 3 months after completing the final session. Hair removal was performed without topical anesthetic.
Laser System
A 755-nm diode laser was used with a spot size of 1.5 cm2 and with a contact cooling system (Soprano ICE, Alma Lasers, Caesarea, Israel). According to the technical data provided by the manufacturer, the laser applied in in-motion mode (Super Hair Removal, SHR) works by gradually heating the dermis to a temperature that effectively damages the hair follicles and prevents regrowth, while avoiding injury to the surrounding tissue. Short impulses at a rapid rate of repetition are delivered deep into the dermis, achieving high average power and therapeutically effective heat build-up, with virtually no pain, according to the manufacturer’s reports. As per the manufacturer’s information, the sweeping in-motion tech-nique of moving the applicator repeatedly over the treatment areas ensures full coverage while ICETM technology cools the skin surface, thereby preventing superficial burns and allowing for virtually painless yet highly effective hair removal.
755 NM DIODE LASER: CLINICAL ASSESSMENT
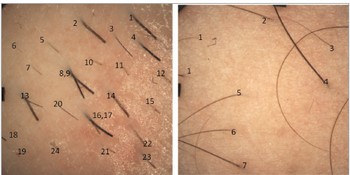
Fig. 1. Procedure for the counting of hair roots per square centimeter, before and after the treatment, based on the images obtained using the camera of the Vivascope confocal microscope.
The following theoretical guidelines were taken into account when applying the treatments:
(1) Conventional technique (Hair Removal, HR): suitable for fine or thick hair in patients with phototypes I–IV. The equipment makes it possible to apply fluences of between 1 and 120 J/cm2 and pulse frequencies of between 1 and 3 Hz. The average fluence used on the sample was 22.5 J/cm2, with a range of 18–32 J/cm2.
(2) In-motion technique (Super Hair Removal, SHR): suitable for all hair types in patients with phototypes III, IV, V, and VI, using fluences between 5 and 20 J/cm2, a pulse frequency of 10 Hz, a pulse duration of 20 ms, and a delay between pulses of 80 ms. In this study, a total accumulated energy of 133 J/cm2 was used for thick hair and 160 J/cm2 for fine hair, with a total average energy of 143 J/cm2. These energy levels were achieved by programming low fluences (8–12 J/cm2), with a high pulse frequency (10 Hz) and multiple passes, until the scheduled energy for each area was attained.
(3) Stacking technique (static hair removal in bursts): suitable for removing hair from well-defined areas, such as between the eyebrows or the upper edge of the eyebrows. Fluences of 4–6 J/cm2 were applied, with a number of programmable pulses and a pulse frequency of 10 Hz in bursts. Two pulses per burst were chosen, reaching a total accumulated energy of 39 J/cm2.
Assessment of Efficacy and Adverse Effects
An area of 10*10 cm was selected in the majority of treated areas for counting the number of hairs per cm2.On the face and in demarcated areas, rectangular or smaller areas were selected. ’Before and after’ photographs of the depilation areas were taken using a Nikon Coolpix P50, 12.1-megapixel camera (Nikon, Tokyo, Japan), and micro-scopic images were taken using the camera of the Vivascope 1500 confocal microscope (MAVIG, Munich, Germany), which records high-definition images and makes it possible to count the number of hairs present per square centimeter. The hair counts before and after treatment were compared using the Mann–Whitney U test. The clearance percentage per square centimeter was calculated as the ratio between the number of hairs after treatment and the number of hairs before treatment * 100, as shown in Figure 1. The clearance of the area in each patient was determined as the average of the assessed square centimeters.
All of the participants were asked to rate their degree of satisfaction with the results on a scale of 0–10.
Adverse effects were recorded in the patients’ clinical histories and, in the first session, patients were also asked to rate the degree of pain as follows: Nil, Light, Moderate, Severe, or Very Severe.
RESULTS
All of the patients completed the treatment. Four participants who could not attend within the assigned time periods and who cited personal reasons not connected to the trial, were excluded from the study.
Hair removal was effective with the three tested treatment techniques (P < 0.0001). The average clearance achieved using the conventional (HR), in-motion (SHR) and stacking techniques were 75.5% (r =58–94%), 70.1%(r =63–91%), and 41.9%, (r =33–46%), respectively. No significant differences were detected between the clear-ance observed in patients with previous hair removal treatments and patients receiving treatment for the first time, nor were differences observed between light and dark phototypes. No significant differences in terms of clearance were found between the conventional and in-motion techniques, whereas the stacking technique proved to be less effective.
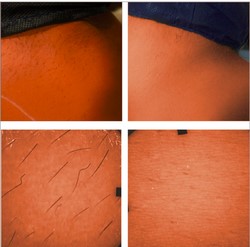
Fig. 2. Example of hair removal using the in-motion method (SHR). The bikini line area on a woman with phototype V, with brown medium thickness hair. The total clearance percentage was 91%.
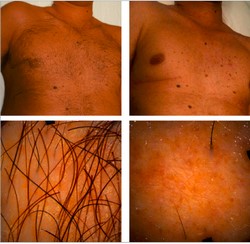
Fig. 3. Example of hair removal using the conventional method (HR). The chest area of a man with phototype IV, with dark thick hair. Total clearance percentage was 94%.

Fig. 4. Example of hair removal using the stacking method. The area between the eyebrows on a man with phototype III, with dark medium thickness hair. The total clearance percentage was 46%.
Some of the results obtained in patients with phototypes III–V treated using the three methods are shown in Figures 2–4; clearances of over 90% were achieved using both the conventional and the in-motion technique.
The degree of patient satisfaction on a scale of 0–10 was 7.4 (r =4–10) for the conventional technique, 8.1 (r =5–10) for the in-motion technique, and 6.8 (r =5–8) for the stacking technique.
No unexpected adverse effects were observed. Erythema and perifollicular edema were observed in all patients (normal events in laser hair removal). Of a total of 224 sessions carried out, there were two instances of first-degree burns, and one instance of a superficial second-degree burn, on thighs (HR mode), beard (stacking mode) and bikini line (SHR mode), respectively. This represents an incidence of burn injuries of 1.33% in all the procedures performed. No dyschromia, hypopigmentation, or other adverse effects associated with photoepilation were observed.
The treatments were well tolerated. The degree of pain reported during the first treatment session for each of the three methods used is shown in Table 1.
TABLE 1. Degree of Pain Reported by the Interviewed Patients in the First Session and Percentage of the Samples for Each of the Treatment Methods

DISCUSSION
The characteristics of the new equipment, as well as its effectiveness (efficacy under the conditions we used), have been very positive for the clinical research team, which is aware of the limitations and problems associated with hair removal and with the demands of patients. We consider the subjective efficacy scores expressed by the participants to be clearly satisfactory, taking into account that these tend to be demanding patients and that a painless, rapid and perfect solution for removing all types of hair has yet to be found.
The conventional and in-motion techniques achieved high clearance levels, with a good efficacy/safety profile, both in first-time patients and in patients who had been treated before. The personalization of the dosimetries and of the type of treatment chosen enabled similar efficacy levels to be achieved in cases with a wide range of difficulty levels. The difficult cases in terms of anatomical areas, skin phototype, and hair characteristics were resolved as satisfactorily as the cases that do not usually present problems. This was possible thanks to the personalization of the treatments and to the safety that the in-motion technique appears to offer for dark phototypes, although our sample of phototype V was very small.
On average, we consider that the clearances achieved were good in the context of the literature [7–11], and very good in comparison with our previous experience with other equipment [6,12–14]. The efficacy percentages obtained appear lower than those achieved by Paasch et al. in a single patient with more suitable hair removal characteristics, using lower (and less painful) fluences, with the same laser [7]. Paasch observed a clearance of 91.6% using the in-motion technique and 88.8% using the conventional technique. Our study obtained relatively lower averages, which do not highlight the best cases. The images shown in the photographs are of results from the higher end of the efficacy range.
It should also be noted that comparing clearances from very different studies, using different patients and methodologies, presents many limitations. For example, Jin et al. found reductions or clearances of 29.1% after four sessions using the 755-nm alexandrite laser [8], whereas Khouri describes clearances of up to 70.3% after just three sessions using the same laser [9]. Even in our study, using the same hair-counting methodology, the observed vari-ability between subjects was relatively wide.
The concept of using low fluences at a high average power with a multiple pass in-motion technique was introduced for the 810-nm diode lasers, leading to a dramatic decrease in therapy-related pain, less discomfort and good effi-cacy [15–17]. The pain experienced by our patients was more significant than in the case presented by Paasch et al. [7] because higher fluences were required to achieve the results obtained. However, we should stress the good tolerance of the in-motion method, in which the level of pain was comparable when applying much higher total accumulatedenergythanwiththe conventional method.
The 755-nm wavelength, with a greater affinity for melanin than the 810-nm wavelength proved to be capable of eradicating fine and slightly pigmented hair, or miniaturized hair, in phototypes III, IV, and V when applied using the in-motion method. This therapeutic window is not well covered by other equipment available on the market. The results using the SHR method suggest that low fluences (8–12 J/cm2) administered using a high pulse frequency (10 Hz) will enable a gradual, destructive heating of follicles, with little risk of thermal injuries, also potentially in phototypes V and VI. Hair survival and growth would be affected by the high energy deposit per surface unit, which is achieved by the multiple laser pulses and the constant movement of the handpiece on the treated surface. The shortage of phototype V subjects and the absence of phototype VI subjects in the researched sample do not allow us to provide more information in this regard.
In our clinical experience, we have found that residual hair responds poorly to the 810-nm diode laser and that, when using the 755-nm alexandrite laser, we can only safely achieve fluences of 26–28 J/cm2. Using the new 755-nm diode laser in in-motion mode, the total accumulated energy was 143 J/cm2, which was very high but well tolerated and with a low risk of burns, and was able to remove residual hair from patients previously treated using the 810-nm diode laser and the 755-nm alexandrite laser.
Hair-removal efficacy was lower when the stacking technique was used, probably due to the way in which the pulses were fired in bursts, with lower accumulated energy per treatment area. However, this technique is useful in areas where the in-motion technique is not sufficiently accurate-for hair removal between the eyebrows, the upper edge of eyebrows or the definition of the upper edge of a beard, for example.
These preliminary results suggest that the 755-nm diode laser may be a highly efficacious, versatile, and efficient tool for medical hair removal. The most notable character-istic of this laser is the high energy that can safely be applied to treat difficult cases. Comparative studies are required between the 755-nm alexandrite laser and the 810-nm diode laser to determine potential advantages and disadvantages of this technological innovation. The per-formance of this laser in phototype VI also remains unknown and requires future research.






